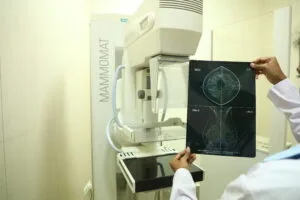
Premarital Health Screening

A premarital test is a test that offers a crucial health assessment of soon-to-be married couples in which they are tested for genetic, infectious and transmissible diseases to prevent any risk of transmitting any disease to each other and their children.
Marriage is considered a remarkable event in a couple’s life, as they plan to start a family, and through which they usher in a new stage in terms of building emotional, social, familial and healthy relationships.
Premarital testing programs should educate couples, providing accurate and unbiased information. Family background, hereditary factors, age, diet, exercise, weight management and addictions all contribute to the bigger picture.
For couples considering marriage, pre-marital screening helps identify potential health problems and risks for themselves and also their offspring. It is vital for couples to be screened in order to aid them to understand their genetics and help them take the necessary precautions or treatments.
Importance of Premarital Screening:
Gauge the positive health status of prospective bride and groom
Detect infectious diseases – Hepatitis B infection, HIV, HCV and other sexually transmitted diseases
Identify carriers of genetic disorders, in order to assess the risk of having children with a severe form of the disease. The couple can then choose whether or not to have an affected child. e.g. Thalassemia, Hemophilia and Sickle Cell Disease
Tests that constitute Premarital Screening:
Routine Investigations – Complete Blood Count (CBC), Complete Urine Analysis and Peripheral Blood Smears to check for normal and abnormal cells. Blood group testing (ABO-RH) is important to screen out the Rh-negative women and counsel them about the risks in pregnancy
Infectious Diseases
– VDRL for Syphilis Testing
– HIV I & II
– Hepatitis-B Screening
– Hepatitis-C Virus
Infectious diseases like HIV, Hepatitis B Virus (HCV), Hepatitis B Virus (HBV), Syphilis and Sexually Transmitted Disease (STD).
Among the blood-borne viruses transmissible through the parenteral route, by blood transfusion, as well as, by sexual intercourse, Human Immunodeficiency Viruses (HIV), Hepatitis B Virus (HBV) and Hepatitis C Virus (HCV) are important and have several implications.
Pre-marital Screening also helps rule out carrier status of potentially life-threatening infectious diseases like HIV and HBV. The World Health Organization (WHO) notes that HBV is 50 – 100 times more infectious than HIV. HBV can be passed from mother to baby during birth. Therefore, it is imperative to safeguard yourself from these potentially life-threatening diseases with simple screening.
Not only do they establish asymptomatic persistent infections, but they also cause significant morbidity and mortality when transmitted through transfusion of blood and blood products.
Failure to diagnose and treat STDs at an early stage result in serious complications and sequelae, including infertility, fetal wastage, ectopic pregnancy, cancer and death.
Genetic Tests
Doctors usually go for culture-based genetic screening. Depending on your family history and ancestry, different tests are designed for different disorders like thalassemia
The tests are especially referred to in ‘consanguineous marriages’ or relationships by blood or common ancestry, in which the chances of offspring inheriting a recessive allele for a disease are increased. The closer the relationship, the greater the risk
Genetic tests are done by analyzing small samples of blood or body tissues
Thalassemia
Thalassemia is an inherited blood disorder (passed from parents to children through genes). Anemia is a disorder in which your body doesn’t have enough normal, healthy Red Blood Cells (RBC).
When thalassemia is called “alpha” or “beta,” it refers to the part of hemoglobin that isn’t being made. If either the alpha or beta part is not made, there aren’t enough building blocks to make normal amounts of hemoglobin. Low alpha is called alpha thalassemia. Low beta is called beta thalassemia.
When the words “trait,” “minor,” “intermedia,” or “major” are used, these words describe how severe the thalassemia is. A person who has thalassemia trait may not have any symptoms at all or may have only mild anemia, while a person with thalassemia major may have severe symptoms and may need regular blood transfusions.
What is Thalassemia Minor?
People with a thalassemia mutation only in one gene are known as carriers or are said to have thalassemia minor. Thalassemia minor results in no anemia or very slight anemia. People who are carriers do not require blood transfusion or iron therapy unless proven to be iron deficient.
What is Thalassemia Major?
Children born with thalassemia major usually develop the symptoms of severe anemia within the first year of life. Lacking the ability to produce normal adult hemoglobin, children with thalassemia major:
– Are chronically fatigued
– Fail to thrive
– Can show growth abnormalities
If both parents carry thalassemia minor, their children may have thalassemia minor, or they may have completely normal blood, or they may have thalassemia major. In each pregnancy there is a one in four (25%) chance that their child will have normal blood, a two in four (50%) chance that the child will have thalassemia minor or a one in four (25%) chance that the child will have thalassemia major.
Signs, symptoms and complications of thalassemia:
The symptoms of thalassemia vary depending on the type of thalassemia. Symptoms will not show until the age of 6 months in most infants with beta thalassemia and some types of alpha thalassemia. Common symptoms include: Weakness, fatigue, pale skin, drowsiness, delayed growth, shortness of breath, leg cramps, and jaundice. Complications include: greater risk of infections, iron overload in the body, gallstones, enlarged spleen and organ dysfunction.
When to get tested for Thalassemia
If you have a family history of the condition or your partner is a carrier
Every individual about to get married must undergo a complete pre-marital check-up and thalassemia testing must be a part of it
Screening during pregnancy (10-12 weeks) by chorion villous sampling, if both parents are thalassemia minor, to check if a baby is at risk of being born with thalassemia
How is thalassemia diagnosed?
– Complete blood count (CBC) Determines the number, size and shape of red blood cells present and the quantity hemoglobin is in them.
– Hemoglobin electrophoresis, the gold standard in the screening and diagnosis of thalassemia: This test detects abnormal forms of hemoglobin as seen in thalassemia.
– Genetic tests: These tests are used to help confirm genetic mutations associated with thalassemia and confirm the presence of the disorder in the alpha and beta globin-producing genes of hemoglobin.
What are the treatment options for thalassemia?
Treatment depends on the type and severity of thalassemia and following therapy options can be chosen by your doctor on a case-to case basis.
– Blood transfusions: Patients with thalassemia major will need a transfusion approximately every 3 weeks
– Iron chelation: Blood transfusions cause an iron overload in the body. Chelation involves removing of this excess iron
– Bone marrow or stem cell transplant: A transplant from a compatible donor is an effective treatment in thalassemia major. Currently, this is the only known cure
– Gene therapy: Scientists are investigating genetic techniques to treat thalassemia. Possibilities include inserting a normal beta-globin gene into the patient’s bone marrow, or using genetic techniques to repair the abnormally functioning genes
What are the socio-economic implications of thalassemia on patients and their families?
– The mental, financial and social burden of going through monthly or fortnightly blood transfusions, prolonged medical therapy and the risk of infections and complications that come along with frequent blood transfusions.
– Struggle and difficulty in finding life partners of their choice and a constant social stigma
– Loss of productive hours at work and discrimination at work
– The country’s blood transfusion burden is 2,00,000 units every month
Thalassemia can be prevented!
Birth of Thalassemia major children can only be prevented by knowing the thalassemia status of the parents before the child is conceived. If both parents test positive for the carrier state, they need to be counselled for prenatal diagnosis in the first trimester of pregnancy to know whether the baby is affected or not. If affected, medical termination of pregnancy is advised.
Don’t reject a thalassemia minor individual, get to know your status first!